Making Every Childhood the Beginning of a Healthy, Happy Life
The Texas Center for Pediatric and Congenital Heart Disease continues to expand cardiac care services in Central Texas
Reviewed by: Charles Fraser, Jr., MD
Written by: Ashley Lawrence

Every child and their family deserve the best possible care, and the best has come to Central Texas! With a focus on uncompromising quality, unwavering commitment, and both whole-patient and whole-family care, the Texas Center for Pediatric and Congenital Heart Disease, a clinical partnership between Dell Children’s Medical Center and UT Health Austin, is dedicated to making every childhood the beginning of a healthy, happy life.
Since the Texas Center for Pediatric and Congenital Heart Disease was established in September 2018, the heart center has grown to include multiple specialties and a team of over 200 clinicians and other support staff. Led by Chief of Pediatric and Congenital Heart Surgery Charles Fraser, Jr., MD, who has been part of some of the finest institutions in medicine, the Texas Center for Pediatric and Congenital Heart Disease team provides a multi-faceted continuum of care, coordinating patient care with referring physicians and other care team members to ensure patients receive the highest level of specialized treatment and experience a smooth transition into adult congenital cardiac care.
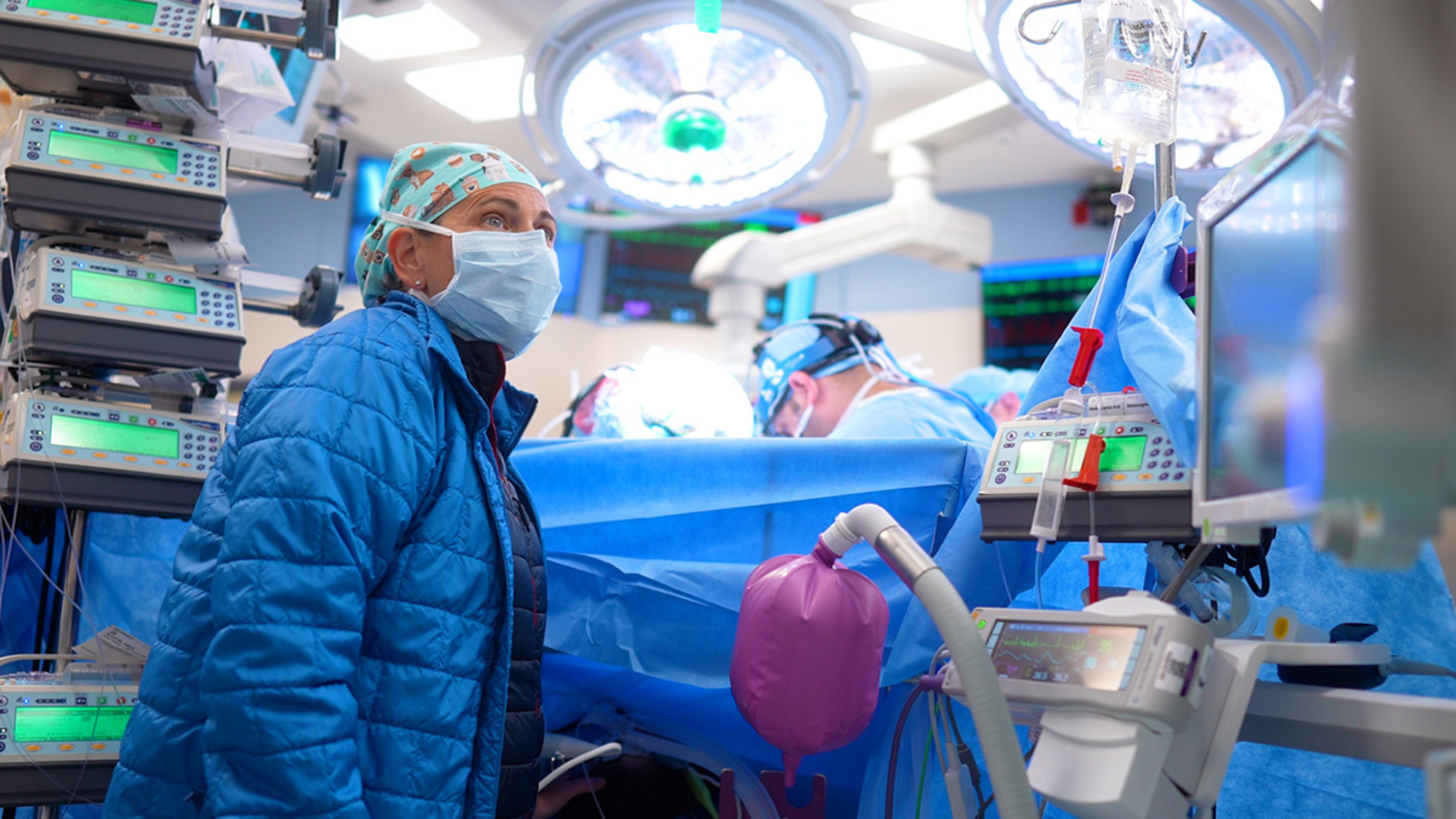
About the Texas Center for Pediatric and Congenital Heart Disease
The Texas Center for Pediatric and Congenital Heart Disease, housed at Dell Children’s Medical Center, diagnoses, treats, and manages the care of children and adults with heart diseases and defects, including aortic coarctation, congenital heart disease, heart failure, pulmonary atresia, pulmonary valve stenosis, single ventricle defects, ventricular septal defects, and more.
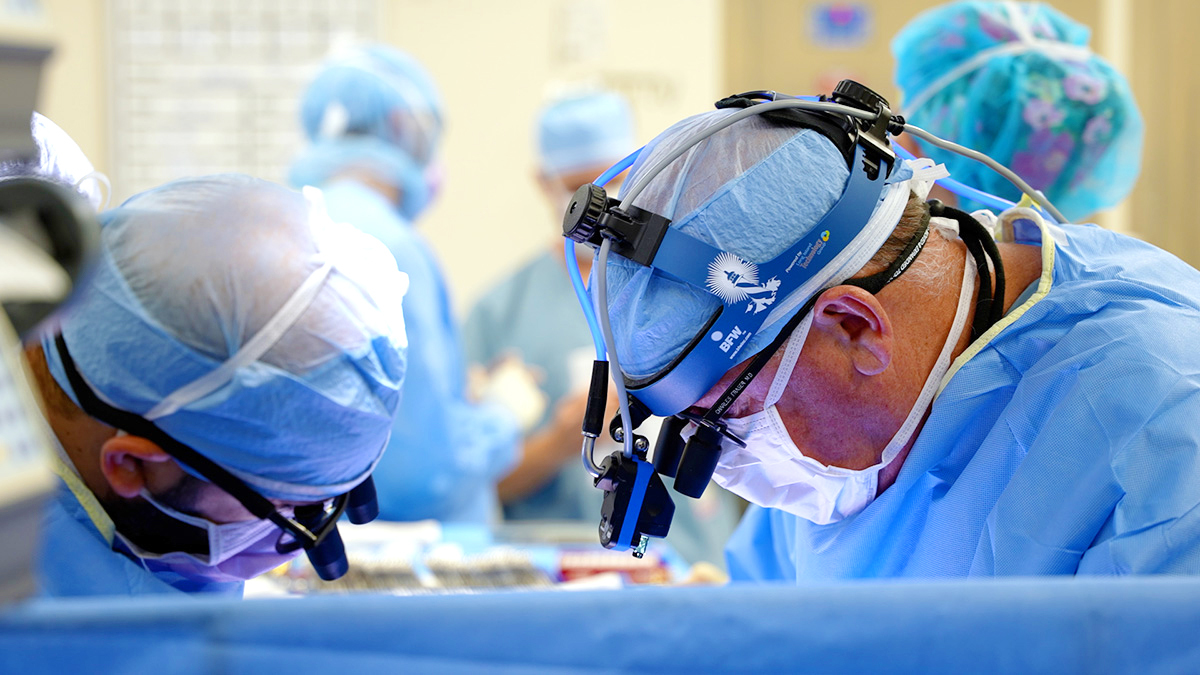
The Texas Center for Pediatric and Congenital Heart Disease care team is capable of treating rare and complex cardiac cases to ensure the best possible outcome for patients and their families. Patients are cared for by a dedicated multidisciplinary care team, meaning patients will benefit from the expertise of multiple specialists across a variety of disciplines. Our board-certified and fellowship-trained pediatric and congenital heart surgeons have extensive experience treating heart diseases and defects in children and adults of all ages and work alongside a team of pediatric and adult cardiac experts.
We also collaborate with our colleagues at the Dell Medical School and The University of Texas at Austin to utilize the latest research, diagnostic, and treatment techniques, allowing us to provide innovative treatment options to patients with heart diseases and defects.
Explore a list of conditions we treat and services we provide.

The Texas Center for Pediatric and Congenital Heart Disease care team includes board-certified and fellowship-trained pediatric and congenital heart surgeons who have extensive experience treating heart diseases and defects in children of all ages and work alongside a team of pediatric and adult cardiac experts, including cardiologists, interventional cardiologists, electrophysiologists, critical care specialists, hospitalists, anesthesiologists, perfusionists, nurses, advanced practice providers, health social workers, psychologists, child life specialists, dietitians, physical and occupational therapists, pharmacists, and more, providing unparalleled care for patients and their families every step of the way.

The Texas Center for Pediatric and Congenital Heart Disease is located in the new Dell Children’s Specialty Pavilion that is connected to Dell Children’s Medical Center. Dell Children’s is the only dedicated freestanding pediatric hospital in Central Texas serving a 46-county area and beyond. The hospital and affiliated locations are outfitted with the latest state-of-the-art technology and organized to support an unmatched level of multidisciplinary care for all patients and their families.
The Pediatric Cardiac Care Unit is a 48-bed inpatient unit at Dell Children’s that is dedicated to delivering highly specialized, whole-person care to infants, children, adolescents, and adults diagnosed with congenital or acquired heart conditions. Patients and families have access to all the resources and amenities Dell Children’s has to offer to make your stay as comforting as possible.
Specialties Within the Texas Center for Pediatric and Congenital Heart Disease
The Texas Center for Pediatric and Congenital Heart Disease is comprised of highly specialized pediatric cardiac care providers who are experienced in providing specific services needed to treat a variety of conditions. Depending on their individual needs, a team is built around the patient and their family to ensure they are receiving the most personalized care.
The Adult Congenital Heart Disease Program diagnoses, treats, and manages the care of adults with congenital heart disease. Our team provides a multi-faceted continuum of care, coordinating patient care with referring physicians and other care team members to ensure patients receive the highest level of specialized treatment. We are dedicated to helping adults with congenital heart disease navigate their lifelong journey while mitigating disability and optimizing their health.
The Cardiac Fetal Program diagnoses, monitors, and manages the care of babies diagnosed with heart problems in utero. Heart problems can include congenital heart disease, heart rhythm problems, or other problems that affect the fetal heart. Advances in prenatal care, such as advanced imaging and testing, have allowed for many heart problems to be detected as early as 12 weeks of gestation. If your baby has been diagnosed with a possible congenital heart problem, the Cardiac Fetal Program care team will work with you to ensure that you understand your baby’s problem, treatment options, and plans for delivery as well as help you better understand the impact that your baby’s problem with have on you and your family in the short, mid, and long term. Our team will also inform all the necessary care team members of your baby’s diagnosis to ensure everyone is prepared for your baby’s arrival.
The Cardiac Neurodevelopmental Follow-Up Clinic tracks, monitors, and manages the development of children with congenital heart disease who undergo surgical intervention as infants. Children with complex congenital heart disease are at higher risk for neurodevelopmental disabilities than other children. This program detects and treats developmental delays with the goal of optimizing each child’s development. Developmental delays may include mild cognitive impairment, oral-motor discoordination, expressive speech and language differences, impaired visual-spatial and visual-motor skills, attention-deficit/hyperactivity disorder (ADHD), learning disabilities, and more. The Cardiac Neurodevelopmental Follow-Up Clinic provides expert evaluation and diagnosis as well as integration of caregiver assessment in which families record and share their own observations related to their child’s development. This allows for early intervention and care coordination between caregivers and experts across specialties to ensure you are your family are provided with the support you need.
The Coronary Anomalies Program diagnoses, treats, and manages the care of children, adolescents, and adults with anomalous coronary arteries. The coronary arteries are small blood vessels that supply blood to the heart muscle. Malformations can occur in the coronary arteries, potentially depriving the heart of oxygen and nutrients and causing serious side effects or cardiac events. While the vast majority of anomalous coronary arteries are not dangerous, there are a few anomalies that may lead to ventricular arrhythmia, myocardial ischemia, left ventricular dysfunction, and, in some cases, sudden cardiac death.
The Heart Failure, VAD, and Transplant Program diagnoses, treats, and manages the care of children and adults with congenital heart disease, who either have a heart muscle problem or are experiencing heart failure. Our team is comprised of nationally recognized and highly specialized physicians across different disciplines housed in a single cardiac care unit at Dell Children’s Medical Center. With access to expert staff and advanced technology, we provide a wide range of services, from evaluation, testing, and diagnosis to medical management, rehabilitation, surgery, heart transplantation, and more, to give patients and their families the best quality of life.
The Single Ventricle Program diagnoses, treats, and manages the care of children with single ventricle heart defects from prenatal life through adulthood. Single ventricle heart defects consist of a wide range of very complex disorders in which the heart cannot be used to pump the blood to both the lungs and the body. When this occurs, the heart is used only to move blood around the body while the surgical team uses a staged approach to create a path for the blood to flow to the lungs without a pump. These conditions put stress on the single ventricle to pump blood to the lungs and throughout the rest of the body. While we expect that most babies with a single ventricle heart defect will have a procedure at birth followed by a bidirectional Glenn shunt procedure at 4-6 months of age and a Fontan operation at 3-4 years of age, some children will require fewer or more procedures.
Major Accomplishments
In just a few short years, the Texas Center for Pediatric and Congenital Heart Disease has achieved several major milestones. Explore some of their latest accomplishments below to learn more about how the Texas Center for Pediatric and Congenital Heart Disease is continually expanding cardiac care services in Central Texas.


On Tuesday, June 25, 2019, a ribbon-cutting ceremony was held for the opening of the Pediatric Cardiac Care Unit (CCU) within the Texas Center for Pediatric and Congenital Heart Disease. The CCU is a 48-bed inpatient unit that includes state-of-the-art technology and is the first and only dedicated pediatric cardiac care unit in Central Texas. As a result, more infants, children, adolescents, and adults diagnosed with congenital and acquired heart conditions will be able to receive the most advanced care close to home.

On September 23, 2019, the Texas Center for Pediatric and Congenital Heart Disease successfully implanted its first mechanical heart device in a pediatric patient in Central Texas. On September 18, 2019, 12-year-old Grace Jennings suffered from cardiac arrest and underwent CPR by Dell Children’s Hospital staff for nearly two hours to save her life. Five days later, the Texas Center for Pediatric and Congenital Heart Disease performed a 10-hour open-heart surgery to implant a left ventricular assist device (LVAD) to stabilize her heart function.
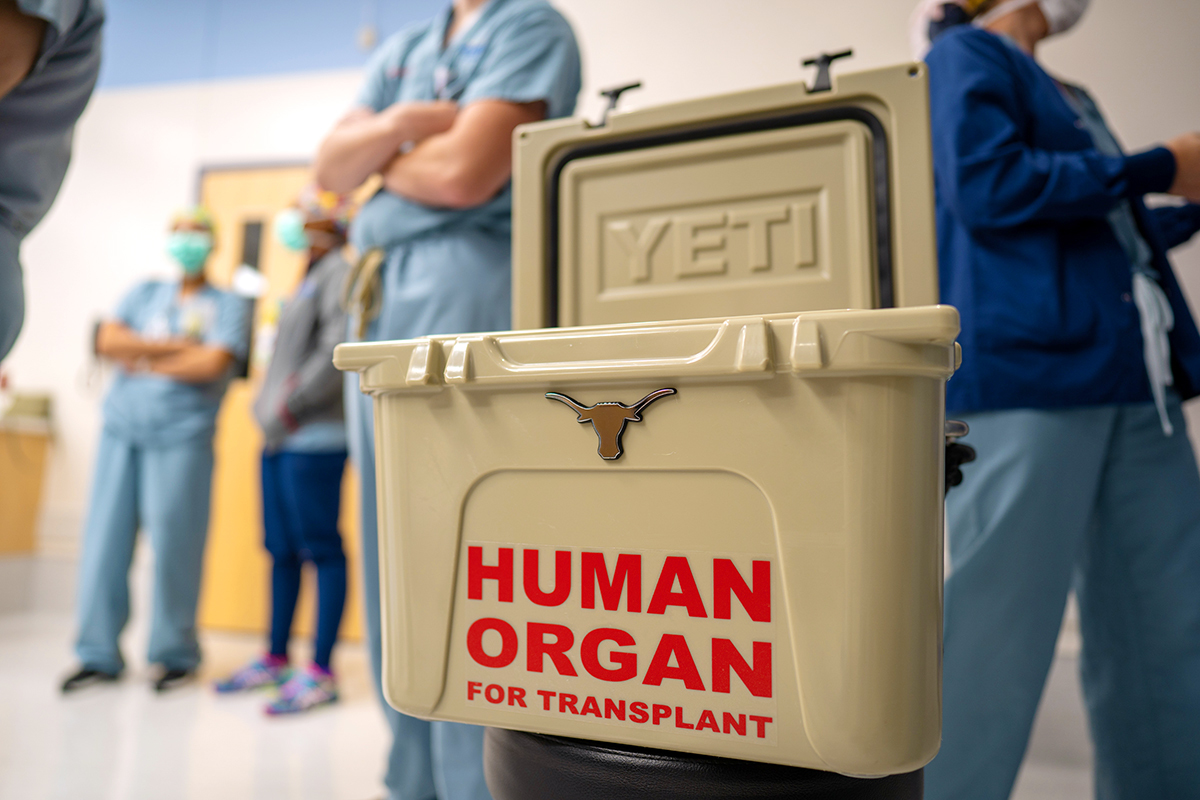
On Friday, July 31, 2020, the Texas Center for Pediatric and Congenital Heart Disease announced the opening of the Heart Failure, VAD, and Transplant Program, the first pediatric heart transplant program in Central Texas. The establishment of the Heart Failure, VAD, and Transplant Program means patients and their families no longer have to travel out of town for this life-saving complex surgery, and they will be better supported throughout their lifetime journey with congenital heart disease.

On Saturday, October 3, 2020, the Texas Center for Pediatric and Congenital Heart Disease successfully performed its first heart transplant at Dell Children’s Medical Center, providing 18-year-old Gerardo Ramirez, Jr. with a lifesaving heart transplant just in time for his mother’s birthday. On Wednesday, December 23, 2020, Gerardo walked out of Dell Children’s Medical Center after being discharged from his 144-day stay just in time to celebrate the holidays at home with his immediate family.
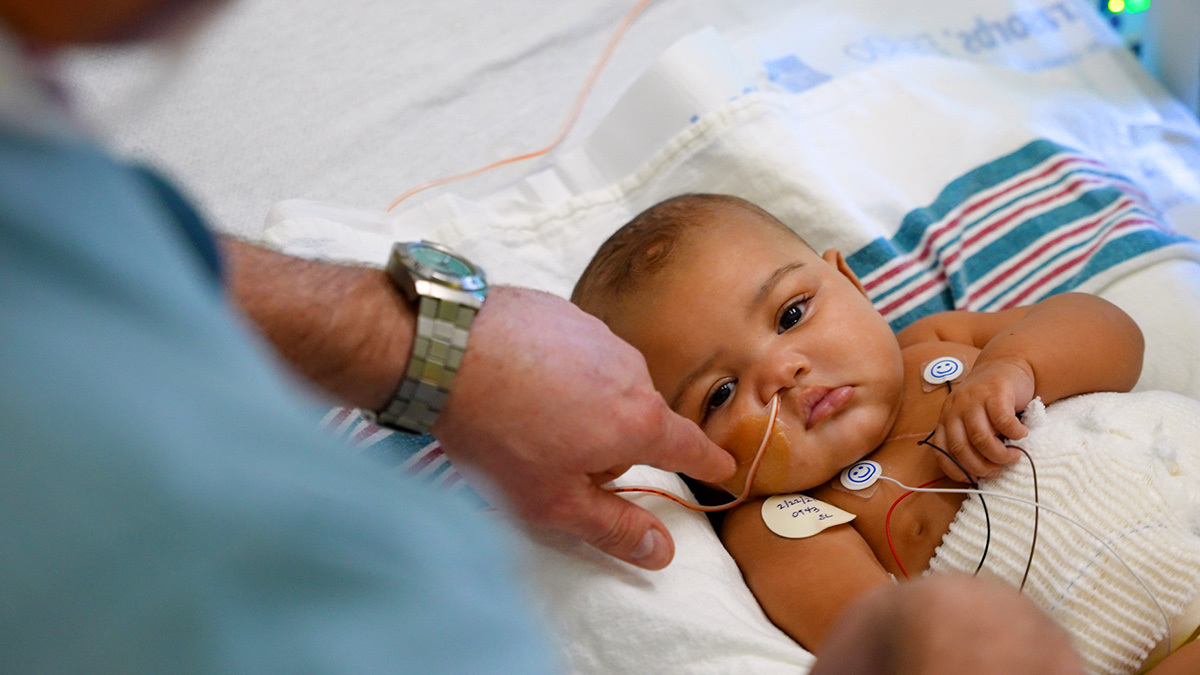
On January 11, 2021, the Texas Center for Pediatric and Congenital Heart Disease successfully implanted its first Berlin Heart ventricular assist device in a pediatric patient, providing 3-month-old Zaria Grace Jackson with a fighting chance while she waited for a heart transplant. On March 25, 2021, Zaria received her heart transplant. After 74 days of recovery, 6-month-old Zaria was discharged on April 19, 2021 and returned home with her family.
On March 3, 2021, the Texas Center for Pediatric and Congenital Heart Disease announced its educational partnership with the Texas Heart Institute in which student perfusionists will now have the opportunity to perform clinical training at Dell Children’s Medical Center. Student perfusionists at the Texas Heart Institute are required to operate the cardiopulmonary bypass machine, commonly known as the heart-lung machine, as well as other equipment associated with open heart surgery during a minimum of 75 cases to fulfill graduation requirements and obtain eligibility to become a certified clinical perfusionist. This education program offered in partnership with the Texas Heart Institute is the first ever clinical affiliation between the Texas Heart Institute and a healthcare system since the school was established in 1962.

On August 13, 2021, the Texas Center for Pediatric and Congenital Heart Disease performed open-heart surgery on its 1,000th patient, 5-year-old Mason Willers, who was born with a partial atrioventricular septal defect, or as Mason’s dad describes it, “a Swiss cheese heart.”

On October 5, 2021, three leading pediatric cardiologists formally joined the Texas Center for Pediatric and Congenital Heart Disease. Each physician also holds a faculty appointment in the Dell Medical School Department of Pediatrics, where they will help shape future generations of leaders in health care. These physicians offer a diverse set of subspecialized clinical care and leadership skills and are leading specialty programs designed to deliver the most advanced medical interventions for both children and adults with congenital heart disease. They will continue to further the strategic mission of the partnership between UT Health Austin, Dell Children’s Medical Center, and the Dell Medical School. Together, these organizations are integrating clinical care, research, and education by building a network of colleagues who focus their energy, expertise, and skills on advancing science and medicine for the benefit of children and families in Central Texas and beyond.
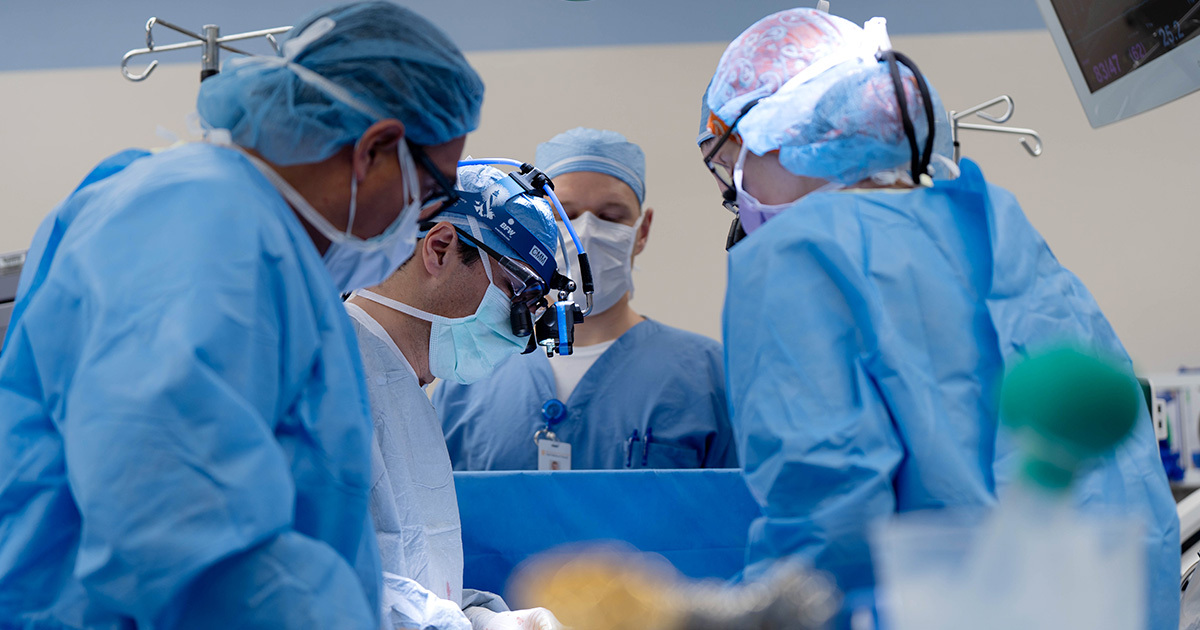
On June 23, 2023, the Texas Center for Pediatric and Congenital Heart Disease successfully performed its first partial heart transplant. A historic first for the State of Texas, this groundbreaking procedure is the seventh recorded instance of a pediatric partial heart transplant performed worldwide.
Meet Some of Our Heart Warriors and Their Families


A few months before Addie’s mom was due to deliver Addie, she received news that her unborn baby girl had heterotaxy syndrome, a condition in which the heart and other organs are not formed correctly or are in the wrong position in the body. Addie’s diagnosis would need to be treated with open-heart surgery soon after she was born. Addie ended up needing two open-heart surgeries across the span of a 9-month hospital stay. When Addie’s surgeon moved from Houston to Austin in August 2018 to help establish the Texas Center for Pediatric and Congenital Heart Disease, Addie’s parents made the decision to follow suit.
Read Addie’s story here.

First diagnosed with a heart condition in 2019, Gerardo had been in end-stage heart failure for almost a year before receiving his heart transplant. He suffered from both hypertrophic cardiomyopathy, a disease in which the heart muscle becomes abnormally thick, making it harder for the heart to pump blood, and Ebstein’s anomaly, a rare congenital heart defect in which the tricuspid valve develops in a way that causes blood to leak backward through the valve and into the right atrium. He was admitted to Dell Children’s Medical Center in August 2020, shortly after the announcement of the opening of the Heart Failure, VAD, and Transplant Program, a specialty program within the Texas Center for Pediatric and Congenital Heart Disease and the first pediatric heart transplant program in Central Texas. Gerardo became the first pediatric patient to receive a heart transplant in Central Texas.

Grace was born with a single ventricle defect, which required multiple cardiac operations early in life. In September 2019, she underwent open-heart surgery through the Texas Center for Pediatric and Congenital Heart Disease after experiencing heart failure and was the first pediatric patient in Central Texas to receive a left ventricular assist device (LVAD), an implanted mechanical pump that supports the circulation and partially replaces heart function in people who have weakened hearts. After waiting 15 months for a donor heart while on the lifesaving mechanical heart pump, Grace received her heart transplant. Grace became the second pediatric patient to receive a heart transplant in Central Texas.

Joaquin began experiencing sudden chest pains and difficulty breathing while playing sports. He was prescribed an inhaler, which temporarily brought relief until his symptoms returned six months later. One evening in September 2018, Joaquin began experiencing intense chest pains while running during baseball practice. After a quick trip to Dell Children’s Medical Center, Joaquin was admitted to the Texas Center for Pediatric and Congenital Heart Disease, where he was diagnosed with an anomaly to the left coronary artery and underwent emergency open-heart surgery to correct the defect.
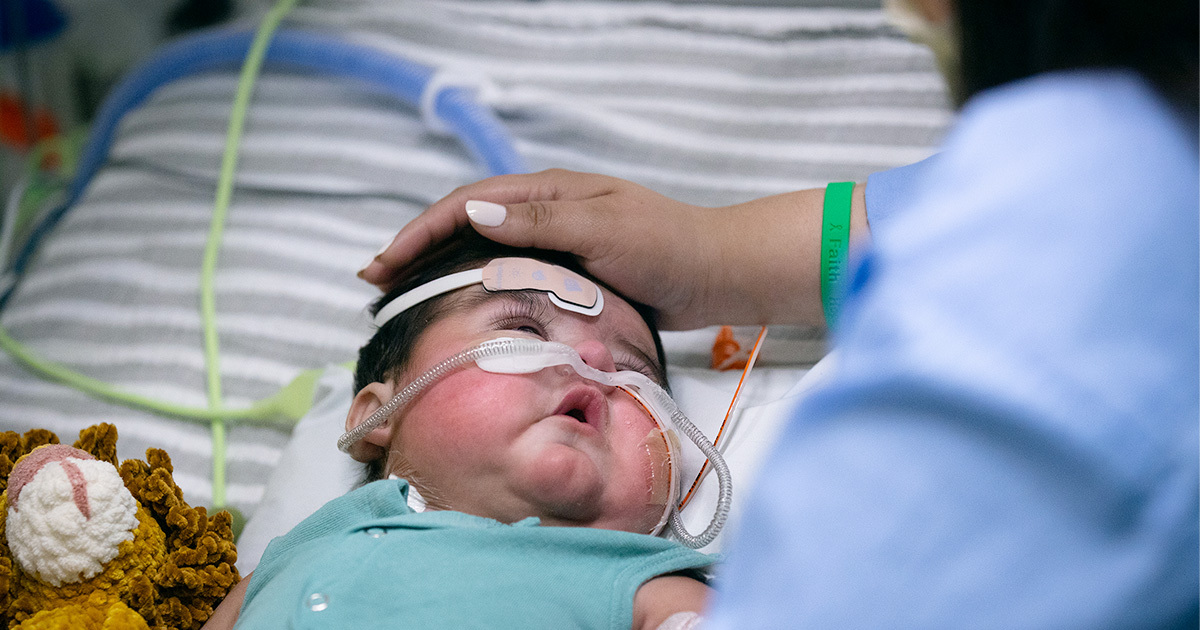
On July 1, 2022, Leo Rodriguez was born with hypoplastic left heart syndrome (HLHS), a rare congenital heart defect that occurs when the left side of the heart is not fully formed during pregnancy. As a result of HLHS, the left side of the heart is unable to support the circulation needed by the body’s organs, which causes the right side of the heart to work harder to pump blood to both the lungs and out to the rest of the body. Typically, babies with hypoplastic left heart syndrome undergo a series of three heart surgeries known as the Norwood procedure, the Glenn procedure, and the Fontan procedure. However, the left side of Leo’s heart had a small cavity that obstructed blood flow in a way that the initial plan to undergo the three surgeries would not restore the heart’s function. Instead, Leo was placed on a heart transplant waiting list. 269 days after birth, Leo received a heart transplant, making him the 20th
pediatric patient to receive a heart transplant through the Texas Center for Pediatric and Congenital Heart Disease and the first to both be born at Dell Children’s and receive a heart transplant there.

Levi was born with a ventricular septal defect, a condition that occurs when the ventricular septum, or the wall that divides the two ventricles (lower chambers) in the heart, does not fully develop during pregnancy, leaving a hole. This small hole allows oxygen-rich blood in the left ventricle to mix with the oxygen-poor blood in the right ventricle, causing added strain on both the heart and the lungs. For children born with a ventricular septal defect, the defect will sometimes close on its own during early childhood as the child develops further and the heart grows larger. In cases such as these, no intervention is needed to fix the problem. However, as in the case of Levi, if the hole does not close fully on its own, surgery is often necessary to prevent the developing of potentially life-threatening health problems later in life. Levi’s parents decided to pursue surgery through the Texas Center for Pediatric and Congenital Heart Disease.
Lincoln was born with congenitally corrected transposition of the great arteries (CCTGA), a rare and complex congenital heart defect in which the two main arteries that carry blood away from the heart (the aorta and the pulmonary artery) are switched. In a normal heart, the left ventricle pumps oxygenated blood into the aorta, which distributes the oxygenated blood to the entire body, while the right ventricle pumps deoxygenated blood into the pulmonary artery, which carries the deoxygenated blood into the lungs for oxygenation. However, in CCTGA, these ventricles are reversed, meaning the stronger left ventricle pumps blood into the pulmonary artery and to the long, while the weaker right ventricle pumps blood into the aorta and out to the rest of the body. In May 2021, Lincoln underwent a pulmonary artery band operation through the Texas Center for Pediatric and Congenital Heart Diease. During the procedure, a band is placed around the pulmonary artery to constrict its diameter and create a partial obstruction to reduce the amount of excessive blood flow into the lungs. This also helps redirect some of the blood back to the body’s systemic circulation, allowing for a more balanced flow of oxygenated and deoxygenated blood.
On August 13, 2021, Mason became the 1,000th patient of the Texas Center for Pediatric and Congenital Heart disease to receive open-heart surgery. Mason was born with a partial atrioventricular septal defect, a heart defect in which a hole exists between the left and right upper chambers of the heart and the valve between the left chambers does not close completely, allowing oxygen-rich and oxygen-poor blood to mix and affecting how the heart and lungs develop. Mason’s parents have been preparing for Mason’s surgery since they learned about their son’s heart defect when Mason’s mother was approximately 18-20 weeks pregnant.

On December 13, 2018, 5-year-old Owen Coulter’s heart stopped beating shortly after he arrived at Dell Children’s Medical Center. In another area of Dell Children’s Medical Center, a pediatric cardiac surgery team within the Texas Center for Congenital Heart Disease was preparing for a scheduled procedure on a patient of their own. An extracorporeal membrane oxygenation (ECMO) machine was on standby in case it was needed during the cardiac surgery team’s procedure. ECMO is a cardiac bypass technology in which a patient’s body is oxygenated without their blood needing to pass through the lungs or heart. ECMO can provide prolonged life support during procedures when a patient’s heart needs to be stopped, but it is rarely used in emergency room situations and had never before been used in an emergency at Dell Children’s. Owen was hooked up to the ECMO machine while teams of five providers rotating every two minutes continued to administer CPR. After undergoing 90 minutes of CPR, Owen regained his heartbeat.

On March 21, 2022, Rubi was diagnosed with Trisomy 13, a rare genetic condition associated with high mortality rates, a range of congenital abnormalities, and severe physical and cognitive impairment. A referral to a pediatric cardiologist confirmed a of tetralogy of Fallot, a rare condition in which a combination of four structural heart defects (overriding aorta, pulmonary stenosis, right ventricular hypertrophy, and ventricular septal defect) occur at once, causing oxygen-poor blood to flow out of the heart and into the rest of the body. Rubi’s parents were met with some resistance when various aspects of Rubi’s health couldn’t be addressed until her heart was fixed. Finding a heart surgeon to take on Rubi’s case was seemingly impossible until Rubi’s parents were connected with the Texas Center for Pediatric and Congenital Heart Disease. On December 21, 2022, Rubi was strong enough to undergo open-heart surgery. Once Rubi’s heart was repaired, Rubi’s parents were able to revisit Rubi’s path to healing and move forward with other surgeries.

On January 19, 2023, Sabine suffered a cardiac arrest due to a coronary artery anomaly, a rare congenital heart anomaly in which the left coronary artery emerged from the right side of the aorta and traveled inside the wall of the aorta before emerging. This caused the segment of the coronary artery inside the wall to become compressed during exercise, cutting the blood supply off from the heart. After 22 minutes of CPR, Sabine’s heartbeat returned, and she was air flighted to Dell Children’s Medical Center and rushed to the Cardiac Care Unit within the Texas Center for Pediatric and Congenital Heart Disease, where she underwent open-heart surgery. The actions of Sabine’s father, her soccer coach, the Austin Police Department, Travis County EMS, the Austin Fire Department, STAR Flight, and Dell Children’s Medical Center all contributed to the chain of survival and played a vital role in Sabine’s successful recovery.

On January 8, 2021, Zaria arrived at Dell Children’s Medical Center emergency department, presenting symptoms and signs of heart failure. After discovering her heart was enlarged, staff quickly admitted Zaria to the pediatric cardiac care unit. As her cardiac condition rapidly deteriorated, the Texas Center for Pediatric and Congenital Heart Disease care team determined Zaria’s best chance for survival was the implantation of a Berlin Heart while she awaited a heart transplant. Zaria became the third pediatric patient to receive a heart transplant in Central Texas.
“These are some of the strongest people we’ve had the privilege of knowing.” – The Texas Center for Pediatric and Congenital Heart Disease Care Team
For more information about the Texas Center for Pediatric and Congenital Heart Disease, please call 1-855-324-0091 or visit here.