About Glaucoma
Glaucoma is a term used to describe a group of diseases that damage the optic nerve, which is responsible for transmitting visual information to your brain. Damage to the optic nerve can lead to irreversible blindness. A leading cause of irreversible blindness in the United States, glaucoma affects more than 3 million patients per year. There is currently no cure for glaucoma, but when identified early, it can be managed medically and surgically by a glaucoma specialist to preserve your vision and prevent permanent vision loss.
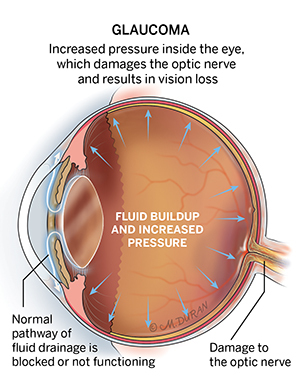
Types of Glaucoma
While there are several types of glaucoma, open-angle glaucoma, and angle-closure glaucoma are the two main types. Open-angle glaucoma occurs when the eye’s drainage canals become clogged over time, causing an increase in eye pressure that damages the optic nerve. Angle-closure glaucoma occurs when the iris bulges forward to narrow or block the eye’s drainage canals, which restricts fluid circulation, causing an increase in eye pressure that damages the optic nerve.
Glaucoma is classified by whether it is caused by another medical condition (secondary glaucoma) or it has no known cause (primary glaucoma).
Examples of types of glaucoma:
- Primary glaucoma:
- Open-angle glaucoma
- Normal tension glaucoma
- Angle-closure glaucoma (closed-angle glaucoma)
- Primary Congenital glaucoma
- Secondary glaucoma:
- Neovascular glaucoma
- Pigmentary glaucoma
- Exfoliation glaucoma
- Uveitic glaucoma
- Traumatic glaucoma
- Secondary Congenital glaucoma
Symptoms of Glaucoma
Most patients with glaucoma, particularly those with open-angle glaucoma, do not exhibit any symptoms. This condition develops slowly and without noticeable change in vision for many years. In advanced cases, loss of peripheral vision, tunnel vision, or patchy blind spots in your peripheral or central vision may occur. Patients with angle-closure glaucoma typically do display symptoms.
Common symptoms of glaucoma include:
- Appearance of “halos” around bright lights
- Eye pain
- Eye redness
- Loss of peripheral vision or tunnel vision
- Nausea or vomiting
- Severe headache
Risk Factors for Glaucoma
Certain people are at greater risk of developing glaucoma.
Risk factors for glaucoma may include:
- Age: While glaucoma can occur at any age, it typically affects those over the age of 60.
- Family history: A family history of glaucoma can increase your risk of developing the condition. Additionally, African Americans, Asians, and Hispanics are at higher risk for developing glaucoma than other races.
- Health history: Glaucoma is associated with a history of diabetes or high blood pressure, low or high eye pressure, past eye surgery or injury, a thin cornea, older age, poor long-distance vision (severe nearsightedness), poor short-distance vision (severe farsightedness), or use of corticosteroids, such as eye drops, pills, inhalers, and creams.
Treating Glaucoma at UT Health Austin
Treatment is dependent on the number of risk factors, the type of glaucoma, and the severity of the disease. Your glaucoma specialist will provide the most current, evidence-based treatment recommendations, which may include medication (eye drops, injections, or oral medications), laser therapy, or surgery. Your first visit often takes 2-4 hours based on the complexity of your case and any in-clinic testing that may be required.
Care Team Approach
At UT Health Austin, we take a multidisciplinary approach to your care. This means you will benefit from the expertise of multiple specialists across a variety of disciplines. Your care team will include fellowship-trained ophthalmologists, ophthalmic technicians, physician assistants, nurse practitioners, social workers, and more who work together to help you get back to the things in your life that matter most to you. We also collaborate with our colleagues at the Dell Medical School and The University of Texas at Austin to utilize the latest research, diagnostic, and treatment techniques, allowing us to identify new therapies to improve treatment outcomes. We are committed to communicating and coordinating your care with your other healthcare providers to ensure that we are providing you with comprehensive, whole-person care.
Learn More About Your Care Team
Mitchel and Shannon Wong Eye Institute
Health Transformation Building, 1st Floor
1601 Trinity Street, Bldg. A, Austin, Texas 78712
1-833-UT-CARES (1-833-882-2737)
Get Directions